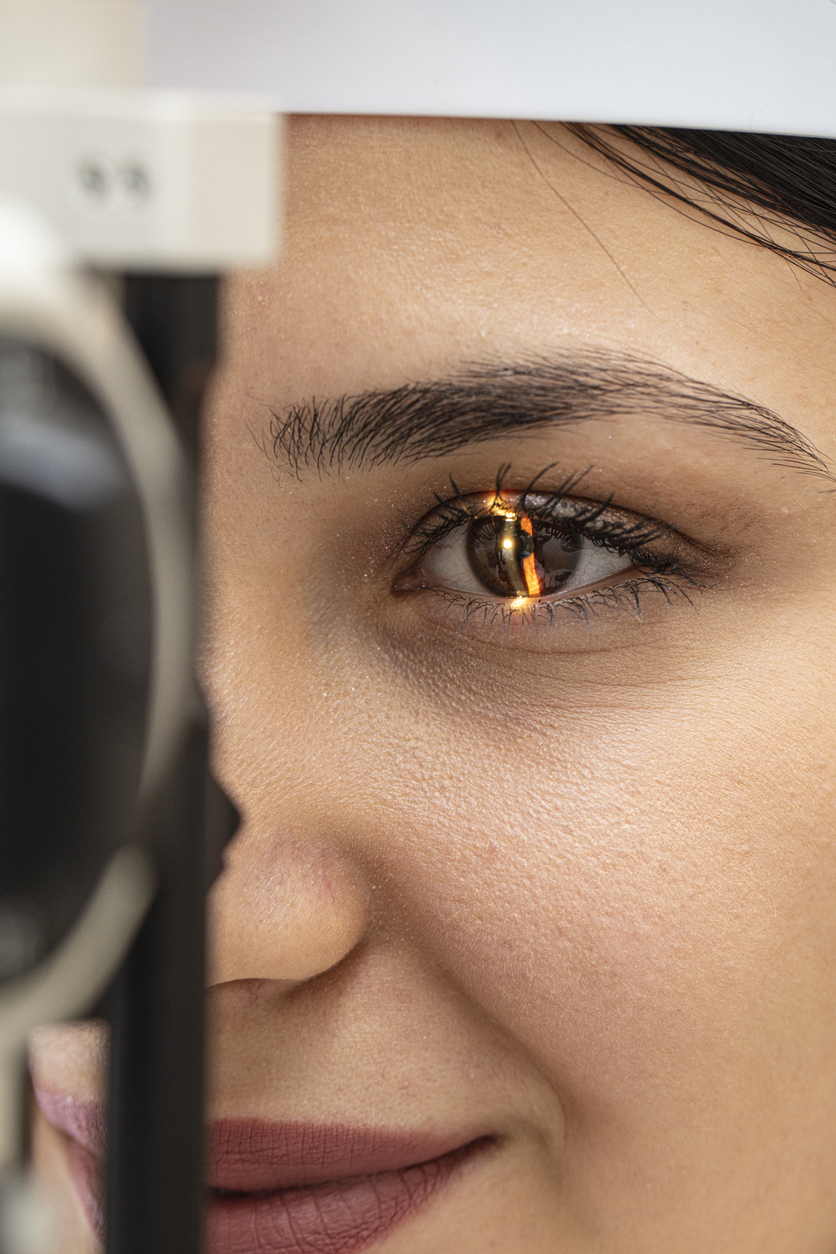
Traditional Cornea Transplant
Understanding Cornea Transplants
The cornea is the very front surface of the eye or the outer surface of the eye and plays a major role in focusing how you see images. If the cornea becomes weak or damaged, serious visual problems may arise. Treating damaged or irregular corneas is something that is routinely done at Eye Consultants of Atlanta. A damaged cornea requires special attention by our specially trained cornea eye surgeons. Often we initially treat the cornea with medication. If the issue with the cornea cannot be corrected with medications, eyeglasses or contact lenses, a corneal transplant or other procedure may be required.

How Does Damage to the Cornea Occur?
Damage to the cornea may arise from various conditions such as hereditary issues, chemical burns, blunt object trauma, and viral or bacterial infections. Conditions that may require a patient to seek a cornea transplant include clouding of the cornea, keratoconus, Fuchs’ dystrophy, irregular corneal surface tissue growths, or corneal scarring due to infection or trauma.