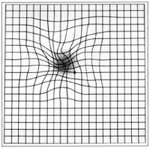
Macular Degeneration

What Is Macular Degeneration?
Age-related macular degeneration (AMD) is the deterioration of the central retina, the macula. The macula is a small, specialized region of the retina and is responsible for central vision. Intact central vision is vital for reading, driving, and recognizing faces. Macular degeneration is a disease process that damages the central vision. It’s one of the leading causes of decreased vision in the United States in patients older than 50 years and the number one cause of blindness in Americans older than 65 years. Many older people develop mild forms of macular degeneration as a part of the natural aging process.
There are different kinds of macular problems, but macular degeneration is the most common macular disorder. Macular degeneration may manifest itself through symptoms such as blurriness, dark areas or distortion in central vision, and at end-stage, a permanent loss of central vision. Macular degeneration usually does not affect one’s peripheral vision. For example, with advanced macular degeneration, people can generally see the outline of a television, yet they may not be able to see the text of the TV screen.
Macular Degeneration Facts
- Those at risk – Individuals older than 60, but macular degeneration can appear as early as age 40. Macular degeneration is the most common cause of severe vision loss among people older than 65, and, as life expectancy increases, the disease is becoming more prevalent.
- The causes of AMD – There is no conclusive proof as to what causes macular degeneration. However, heredity plays a part, and other potential links include UV light exposure, poor vascular status, smoking, and malnutrition.
- The symptoms of AMD – The typical symptoms are distorted vision (typically straight lines or objects appear wavy or crooked), a dark spot in the central vision, and blurring. Later there is loss of central sight.
- What can be done to prevent AMD – Although there is no hard evidence as to how to prevent macular degeneration, there are various steps that may lower risks: proper nutrition, intake of daily vitamins, protection from UV sunlight, smoking cessation, and following nutrition guidelines found in the AREDS 2 (A.R.E.D.S.2) (Age- Related Eye Disease Study 2).
As mentioned, macular degeneration rarely occurs in people younger than 50 years and most commonly occurs in people older than 60 years. Macular degeneration is categorized into two major subsets,”wet” and”dry.”

Dry Form of Macular Degeneration
The Prevention of Macular Degeneration
If you have a family history of macular degeneration or are a cigarette smoker, you may choose to make some lifestyle changes that could help lower your risk for macular degeneration. Listed below are a few tips for macular degeneration prevention.
- Regular exercise
- Weight under control
- Control of blood pressure
- Limiting UV exposure/wear quality sunglasses
- Obtain regular eye exams after the age of 40
- Do not smoke
- Follow AREDS2 nutrition guidelines
The information contained on this page is intended for educational purposes. Any patient with potential retina or eye disease or macular degeneration should consult an Atlanta ophthalmologist before making a judgment on their condition.
For more information on the retina in Atlanta, please contact us today to set up a consultation!


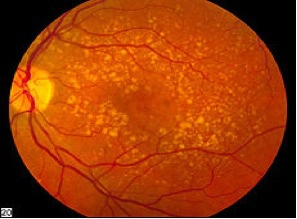


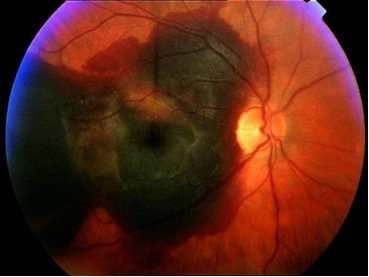
 (National Eye Institute photo)
(National Eye Institute photo)